ChatGPT stirred up pundits and the online world, attracting 1 million users just 5 days after its launch last fall. Even more recently, Microsoft’s chatbot for its Bing search engine has been in the news after generating remarkably human-like conversations. Yet these flashy offerings represent a mere fraction and not necessarily the most substantial of AI’s capabilities and potential.
The potential to apply AI to help reduce costs, create richer member experiences and achieve better health outcomes has caught the imagination of many health plan business leaders. AI applications fall into two broad categories:
- Generative AI algorithms (such as ChatGPT and Google Bard) create new content, including audio, code, images, text, simulations and videos.
- Other AI algorithms, including machine learning (ML), deep learning, natural language processing and computer vision, can analyze data, images and voice and recognize patterns/segments for better decision-making, process optimization and significantly improved customer experience.
With generative and other types of AI algorithms, health plans can automate tasks, increase productivity, generate new ideas and solutions to complex problems and more. AI will increasingly provide the architecture on which health plans can base their operations and member engagement.
Transforming Health Plan Operations with an AI-First approach
AI may be deployed in almost all segments of a health plan’s value chain. It provides ample opportunity for health plans to upgrade their operations, differentiate their offerings and design better member experiences. Some key functions where AI will enable health plans to fill capability gaps, manage complexities and mitigate operational challenges are listed below.
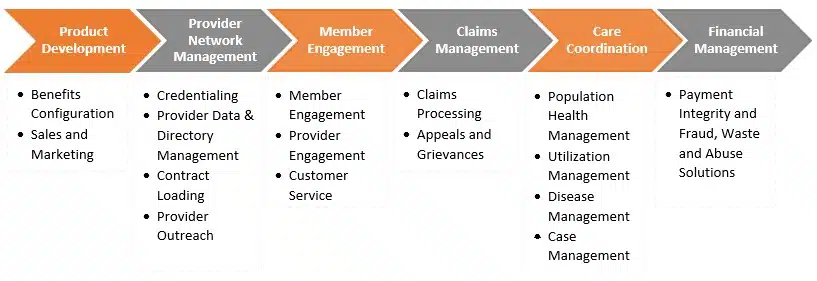
Here’s a look at how an AI-first approach to some of these key functions could change how health plans engage members and deliver services.
AI in sales and marketing. Health plans rely heavily on brokers and agents to provide a personalized customer experience during the health insurance sales process. These brokers and agents use their skills along with industry tools to differentiate their customer service from the competition.
However, generative and other AI algorithms in sales and marketing can take personalization to a whole new level with their potential to better understand a customer’s needs. AI models can analyze members’ historic health and demographic data, identify the most suitable health insurance plan and generate sales content accordingly. Health plans can use these AI capabilities to further personalize plans to a member’s needs. These capabilities should also net such benefits as:
- Increased conversion rates and higher cross-sell/up-sell.
- Reduction in time spent on administrative tasks by agents/brokers.
- Enhanced targeted marketing efforts.
- Discovery of more sales opportunities.
AI-powered customer service agents of tomorrow. Many health plans have implemented conversational AI solutions in their contact center operations to reduce costs and deliver a better experience. Conversational AI automates the responses for the large volumes of daily routine queries health plans receive. However, these solutions usually follow a script and lack natural language processing (NLP) capabilities.
Advanced AI will revolutionize the member engagement model with its large language models and advanced text-to-speech/speech-to-text technology. AI with NLP can generate tailored responses, handle complex queries and even hold more meaningful personalized discussions. This will result in higher member satisfaction and increased efficiency in contact centers, leaving human agents free to give more attention to high-touch calls.
We are not far from a scenario when provider AI bots will request eligibility and claims’ status from a payer’s AI bots.
Accelerated platform configuration enabling faster speed to market. Processes like benefit configuration and contract loading are quite labor intensive and slow down the time to production. Generative AI will produce highly accurate contract and benefit configuration for the core system along with required documentation for members and providers.
AI-enabled automated claims management. Inefficiencies and errors across the claims management process remain the major concern for health plans because these increase operational costs and result in regulatory penalties and interest charges and prove detrimental to member and provider satisfaction. AI is already streamlining the claims management process across its complete value chain. Health plans are deploying decision agents, numerical and natural language data analyzers and predictive models in real-time to derive insights from claims and act on them in sub-seconds. AI-driven models also significantly enhance audit quality by increasing the sample size and focusing on claims with a higher propensity for errors. These AI-powered claims operations will result in the following:
- Faster claims settlement
- Significant reduction in handling times
- Enhanced fraud detection and prevention
- Elimination of duplicate claims
- More accurate payments
- Eliminated late payment interest and penalties
- Improved member and provider experience
Intelligent digitization of payment integrity. Most health plans follow retrospective pay-and-chase models to identify inaccurate payments. This increases operational costs because it requires reworking, reprocessing and recovering claims. AI will enable health plans to switch to real-time accurate payments. Moreover, intelligent analytics will help identify unusual claim submission patterns and quickly detect/prevent fraudulent claims. This will drastically reduce operational costs and increase the efficiency of the system.
Maximizing effectiveness of appeals and grievances with AI. Resolving appeals and grievances (A&G) cases is challenging because it involves coordinating multiple departments. This increases the turnaround time and compliance risk for any A&G case. AI models will provide intuitive and guided workflows for quick and easy understanding of complex cases and further assist in smarter decision-making. They also ensure adherence to regulatory guidelines. This AI-enabled process will result in faster case resolution, higher customer satisfaction and reduced operations cost.
Transforming care coordination to an AI-powered next-gen model. Gaps in care coordination interrupt patient treatment with adverse consequences for health outcomes and the member experience. Deployment of AI across health plan processes will ensure the well-being of members at every step, from care to cure. These solutions can integrate with ongoing digital health initiatives and enhance program effectiveness and health outcomes. Here’s how:
- Utilization Management. AI-driven utilization management will significantly reduce the need for clinicians to manually review authorization requests, a task that adds significant overhead for both plans and providers. AI solutions enable medical necessity determination in near real-time to accelerate decision-making and expedite access to appropriate care.
- Population Health Management. With its machine learning capabilities, AI will provide tailored, personalized recommendations to promote healthy habits and behaviors among health plan members and reduce their need for medical care. Recommendations would include workout regimens, monitoring nutrition/calories, nearby wellness programs, etc., based on the individual’s habits and preferences.
An Imperfect Intelligence
While AI has undoubted value for healthcare, deploying it—especially generative AI—still comes with challenges. Health plans should be aware of generative AI’s growing pains, including:
- Current limited understanding about health plan processes and internal knowledge. Many generative AI models are trained on open internet data. These models do not understand health plan processes, internal language, data sources, workflows and line-of-business-specific nuances. In addition, generative AI models operate as one-size-fits-all. When the model makes a mistake, the only way to correct it is to change the input text prompt. Enterprise customers will benefit from bespoke generative AI models that can learn and be finetuned based on user feedback
- “Hallucinatory” conclusions. Generative AI doesn’t always deliver correct responses. Even more dangerous, the model can sound confidently correct despite being provably wrong. Our experience with generative AI suggests this could break users’ trust.
- Need for integration with key health plan systems and workflows. For AI to drive real value for a health plan, it should integrate with core administrative systems, CRM systems and other enterprise applications. It also should integrate into different workflows, such as claims, A&G, UM, case management, enrollment, credentialing etc., and drive actions across these functions. It will also need real-time information and the context of the constituent for delivering moments that matter. The low-code/no-code Enso platform enables AI models to connect with different systems for claims and revenue cycle management (RCM). As a result, it can turn conversational insights and signals in the data into actions that drive key business outcomes.
Start building AI into operations today
Accessing and integrating high-quality data from various sources, regulation and privacy concerns and the lack of skilled professionals who understand both AI and healthcare remain major concerns. One solution would be for health plans to turn to services companies with the expertise to plug these capability gaps.
Turning to a trusted third-party service provider could enable health plans to adopt AI on a much larger scale across different functions. The service provider could draw on economies of scale to manage complexities, mitigate operational challenges, supply talent and ensure compliant adoption of AI.
Healthcare’s regulatory environment and mandate to do no harm require AI to be deployed with transparency and care. Nonetheless, health plans can turn to AI today to solve operations challenges and begin to build the AI-first operations and engagement architecture that will help them remain relevant and successful in a member-first, digitally driven industry.
For additional information, please get in touch with Deepan Vashi (deepan.vashi@firstsource.com), EVP – Healthcare Payer Practice and Solutions Lead, Solutions Architecture, Firstsource, or contributing authors, Anurag Yadav (anurag.yadav@firstsource.com) AVP – Presales, Solutions Architecture, Firstsource, and Anushka Saxena (anushka.saxena@firstsource.com), Assistant Manager – Presales, Firstsource.










